Blog > Vascular Diseases > Deep Vein Thrombosis and Its Health Complications
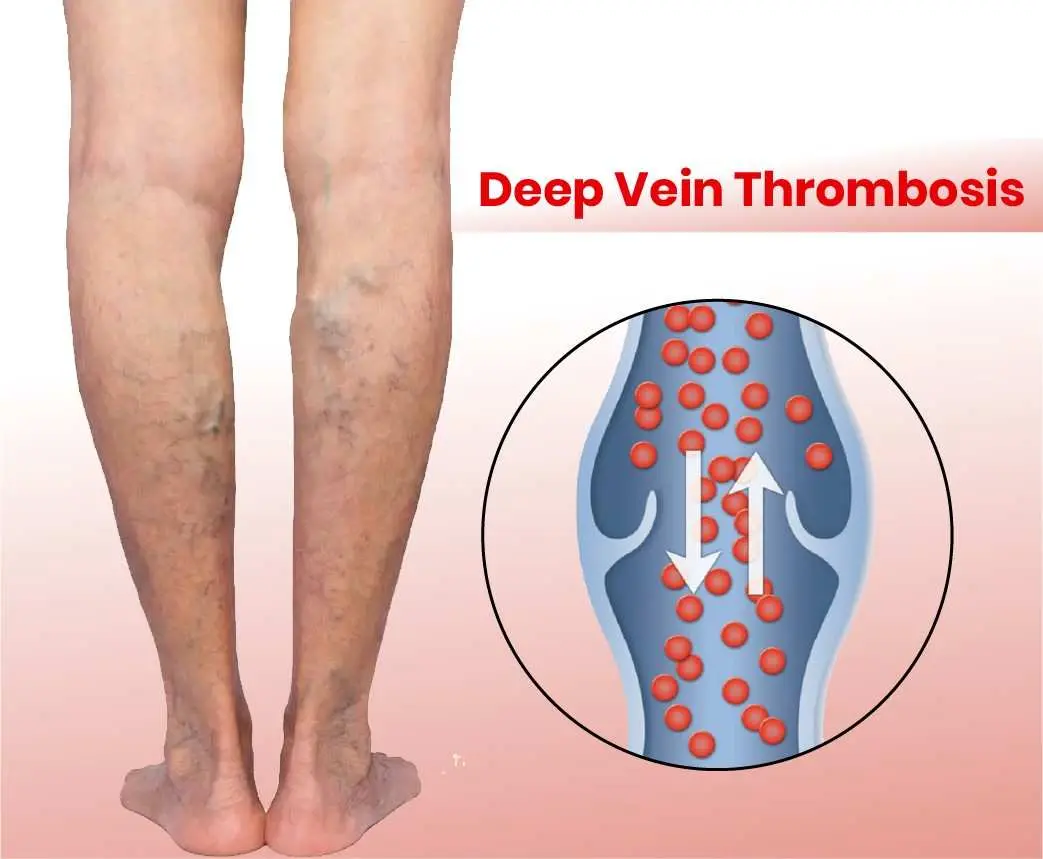
What is DVT?
Deep Vein Thrombosis, abbreviated as DVT and also referred to as venous embolism,
thrombophlebitis, or phlebothrombosis is a medical condition where blood clots (thrombus)
develop in the deep veins of the legs.
DVT occurs as a result of blood pooling in the veins and the neighbouring tissues which act as a
trigger for the blood clotting mechanism. Although DVT can occur in the veins of other body
parts as well, these have been commonly observed in the lower legs, usually between the ankle
and upper calf.
Blood clots in the deep vein thrombosis condition may partially or completely hinder the blood
flow. These may also travel deep within the veins of the pelvis, arms, heart, brain, lungs, etc
and lead to life-threatening medical conditions.
Both Deep Vein Thrombosis (DVT) and Superficial Vein Thrombosis (SVT) are types of
thrombophlebitis but SVT is less dangerous as blood clots are formed in the superficial veins
and not the deep veins. As opposed to SVT which is not related to any serious complications, DVT
requires immediate medical attention or can lead to death.
What causes DVT?
The most common cause of Deep Vein Thrombosis is inactivity. The lesser you move, the poorer is
your blood circulation and this increases the chances of blood clotting by multi-fold.
Blood clots often develop in extended periods of inactivity. If you sit for long periods at your
office desk or undertake elongated travel trips in a flight or car, or frequently binge-watch
movies or web series, you are at a higher risk of developing clumps or blood clots in your
legs.
People who are bedridden, paralyzed, or confined to a wheelchair are also highly likely to
develop blood clots due to their inability to move their legs.
At times, any accident or surgery that causes damage to blood vessels may also lead to blood
clots. Patients who have had orthopaedic surgery, pelvic surgery or abdominal surgery have also
been reported to be suffering from DVT. In some cases, DVT has been diagnosed to be genetic or
because of cancer.
How to diagnose DVT?
DVT is considered dangerous because it is a silent medical condition and difficult to diagnose
by external examination. In most cases, especially when the blood clot is too small in size,
there are no visible symptoms. DVT progresses too fast, thus making it even more difficult for
the patient to identify the symptoms.
The most prominent signs of DVT are swelling, pain, and redness in the affected area. There may
also be a prickly sensation in the legs. These symptoms are usually felt in a single leg.
The damaged area may feel warm and tender, it may also ache more when touched or pressed. The
patient may suffer from shortness of breath accompanied by extreme pain that worsens after
walking or standing.
As the visible symptoms develop only in about 50% of patients, it is wise for patients with a
family history of blood clots to monitor their situation and keep a close eye on the symptoms,
if any.
Is DVT a serious condition?
DVT is a very serious medical condition and often leads to the post-thrombotic syndrome which
causes irreversible damage to the veins and the leg. As many as 25% of DVT patients have been
reported to have suffered from permanent damage to their legs due to blood clotting.
Blood clots in the deep veins can grow bigger, break free, and travel through the bloodstream to
other body parts such as the heart, brain, etc. Thus, DVT can also turn out to be fatal for a
few patients.
As the deoxygenated blood from the veins is returning to the lungs for oxygenation, blood clots
in the deep veins may be pushed to the lungs and can result in pulmonary embolism where the
blood supply to the lungs is partially or fully restricted. This medical condition can lead to
death.
Pulmonary embolism is characterized by chest pain that becomes worse with coughing or deep
breathing, dizziness or fainting, increased pulse rate, and unexplained shortness of breath. If
you notice one or more of these symptoms, you must immediately rush to the nearest
hospital.
How to reduce in-flight risk of DVT?
The risk of developing a blood clot increases substantially during a long flight. This is
because there is limited leg space and your legs usually remain in a cramped position for an
extended duration. Inactivity in a flight restricts the blood flow and thus increases the
likelihood of DVT.
Whenever in a flight, you must move your legs as frequently as feasible. Always opt for an aisle
seat as that has a little extra leg space and allows you to get up and walk around the cabin as
many times as you want. You can also stretch your legs once a while.
You must also try and stand occasionally to flex your leg muscles and improve the blood
circulation in the leg veins. If for some reason you are unable to get up, raise and lower your
heels and keep your toes on the floor to exercise your calf muscles.
Always wear loose-fitting clothes and keep your legs uncrossed during your flight. You can also
buy ergonomic devices that stimulate blood flow when body movement is not feasible. Those who
have already been diagnosed with a venous disorder must use compression stockings to improve
blood flow during long flights or car rides.
How to prevent DVT?
Deep vein thrombosis can be easily prevented by being physically active. By performing moderate
exercises every day or going for a brisk walk, you can maintain good blood circulation and that
can help in preventing blood clots.
Getting up from your office desk once every hour or so will also help the blood to constantly
pump through the body. If at all you are unable to get up, keeping legs elevated will also
improve the blood flow.
You must give up on caffeine and alcohol and instead consume plenty of fluids. Keep your blood
pressure under control. Also, consult your medical practitioner about the suggested use of
compression stockings and any blood-thinning drugs that will help regulate your blood flow.
Always eat clean and maintain a healthy weight. Pickup an outdoor sport and team with your
friends and/or family for an everyday evening session. Walk down the road instead of taking a
cab and always prefer the staircase instead of the escalator or the lift. These are small steps
but make a huge difference to your overall health.
How to treat DVT?
As opposed to the ancient times when surgical procedures were the only feasible way to treat
varicose veins and other venous disorders like DVT, today there are available minimally invasive
and painless procedures that efficiently remove the deep vein thrombus and offer instant relief
from symptoms like swelling and pain.
Dr. Rajah V Koppala at Avis Vascular Centre specializes in the endovenous laser treatment which
is performed as an outpatient procedure under the guidance of a doppler ultrasound scan.
Enjoying a high success rate and a negligible rate of recurrence, this procedure is a highly
efficient and safe treatment for a large variety of venous disorders.
If you have a family history of deep vein clots or have visible symptoms of DVT, do not hesitate
or delay the treatment as it can lead to other medical complications. At Avis Vascular Centre,
we treat 45000+ patients every year and have huge experience in curing even the most critical
cases.
We offer 100% price assurance at the time of admission and have partnered with all major
insurance agencies of India to offer easy Mediclaim assistance to our patients. Even if you
reside outside of Hyderabad, our outstation patient care team can help you with your travel and
accommodation bookings and thus ease your procedure.
Get treated by distinguished interventional radiologists at Avis Vascular Centre, book your
consultation today!