Venous thromboembolism (VTE) is a serious condition that includes both deep vein thrombosis (DVT) and pulmonary embolism (PE). It occurs when a blood clot forms in a deep vein, typically in the legs, and can travel to the lungs, causing a potentially life-threatening PE. Understanding how to prevent VTE is crucial for maintaining vascular health and overall well-being. This blog will discuss practical tips and medical treatments to prevent venous thromboembolism.
Preventing Venous Thromboembolism
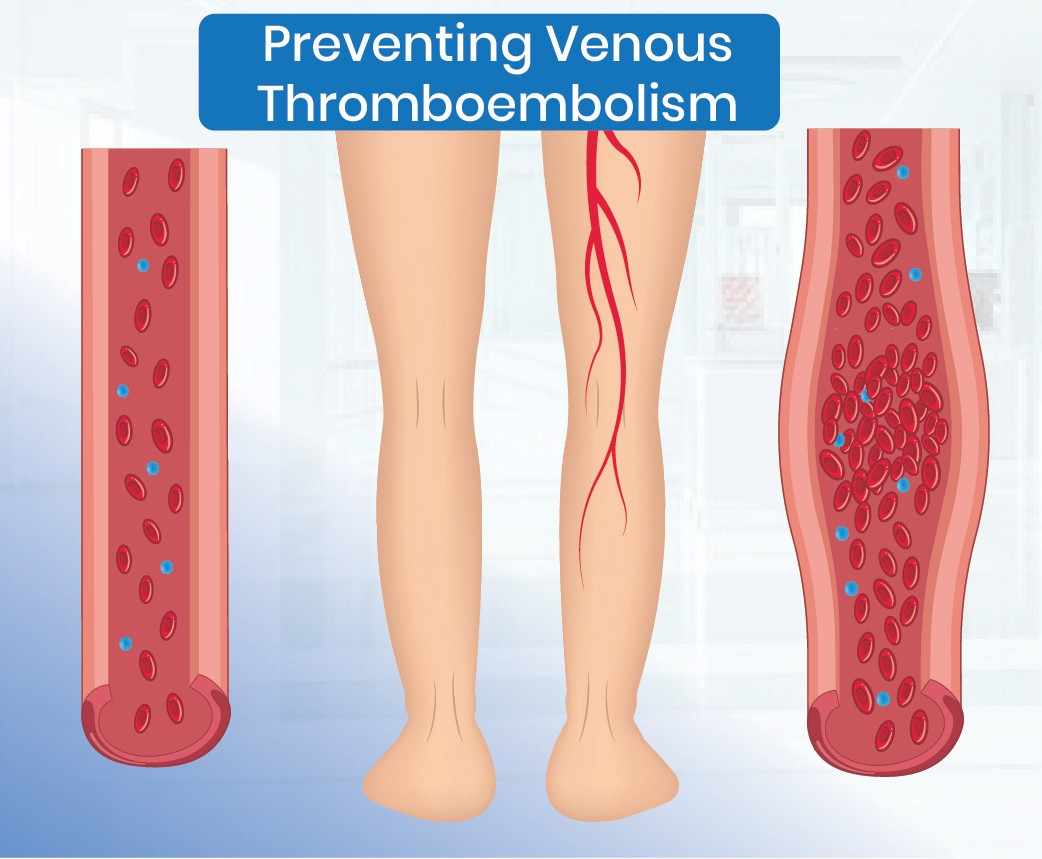
Understanding Venous Thromboembolism
Venous thromboembolism is a condition where blood clots form in the veins. DVT refers to clots
in deep veins, often in the legs, while PE occurs when a clot travels to the lungs, blocking
blood flow. Risk factors for VTE include prolonged immobility, surgery, cancer, pregnancy, and
certain genetic conditions. Symptoms of DVT can include swelling, pain, and redness in the
affected limb, while PE symptoms may include shortness of breath, chest pain, and rapid heart
rate.
Tips for Preventing VTE
1. Stay Active
Regular physical activity is crucial in preventing VTE. Exercise helps maintain healthy blood
circulation and prevents the blood from pooling and clotting. Aim for at least 30 minutes of
moderate exercise most days of the week. Activities like walking, cycling, and swimming are
excellent choices.
2. Avoid Prolonged Immobility
Prolonged immobility, such as sitting for long periods during travel or bed rest after surgery,
increases the risk of VTE. If you are traveling for extended periods, try to stand up, stretch,
and move around every hour. For those on bed rest, perform leg exercises and change positions
frequently to keep the blood flowing.
3. Maintain a Healthy Weight
Being overweight or obese can increase the risk of VTE. Maintaining a healthy weight through a
balanced diet and regular exercise can reduce this risk. Focus on consuming a diet rich in
fruits, vegetables, whole grains, lean proteins, and healthy fats.
4. Stay Hydrated
Dehydration can make the blood thicker and more prone to clotting. Drink plenty of water
throughout the day to keep your blood properly hydrated and flowing smoothly.
5. Wear Compression Stockings
Compression stockings can help improve blood flow in the legs and reduce the risk of DVT. These
specially designed stockings apply pressure to the legs, helping the veins and muscles move
blood more efficiently. They are especially useful during long flights or for individuals who
are bedridden.
Medical Treatments for Preventing VTE
1.Anticoagulant Medications
Anticoagulant medications, also known as blood thinners, are commonly prescribed to prevent VTE.
These drugs work by inhibiting the blood’s ability to clot. Common anticoagulants include
warfarin, heparin, and newer oral anticoagulants like rivaroxaban and apixaban. It is essential
to follow your healthcare provider’s instructions carefully when taking these medications, as
they can have side effects and interactions with other drugs.
2. Compression Devices
Intermittent pneumatic compression (IPC) devices are often used in hospital settings to prevent
VTE, especially after surgery. These devices consist of inflatable sleeves that wrap around the
legs and periodically inflate with air, applying pressure to the veins and promoting blood flow.
3. Inferior Vena Cava (IVC) Filters
In some cases, an IVC filter may be recommended for individuals who cannot take anticoagulants
or have a high risk of PE. This small, cage-like device is inserted into the inferior vena cava,
the large vein that carries blood from the lower body to the heart. The filter traps blood clots
before they can reach the lungs.
4.Periodic Monitoring
For individuals at high risk of VTE, regular monitoring by a healthcare provider is crucial.
This may include blood tests to check clotting times and imaging tests like ultrasounds to
detect clots early.
Preventing venous thromboembolism requires a combination of lifestyle changes and medical
interventions. By staying active, avoiding prolonged immobility, maintaining a healthy weight,
staying hydrated, and using compression stockings, you can significantly reduce your risk of
VTE. Additionally, medical treatments like anticoagulants, compression devices, IVC filters, and
regular monitoring play a vital role in preventing this serious condition. Always consult with
your healthcare provider to develop a personalized plan for VTE prevention, ensuring a healthier
and safer future.
Frequently Asked
Questions
For any unanswered questions, reach out to our support team via email. We’ll respond as soon as possible to assist you.