Blood clots are a significant health issue, and Deep Vein Thrombosis (DVT) is a common and dangerous type. This article delves into the vein problems causing blood clots, focusing on DVT, its potential risks, and preventive measures.
Recognizing the Signs of DVT Blood Cloths
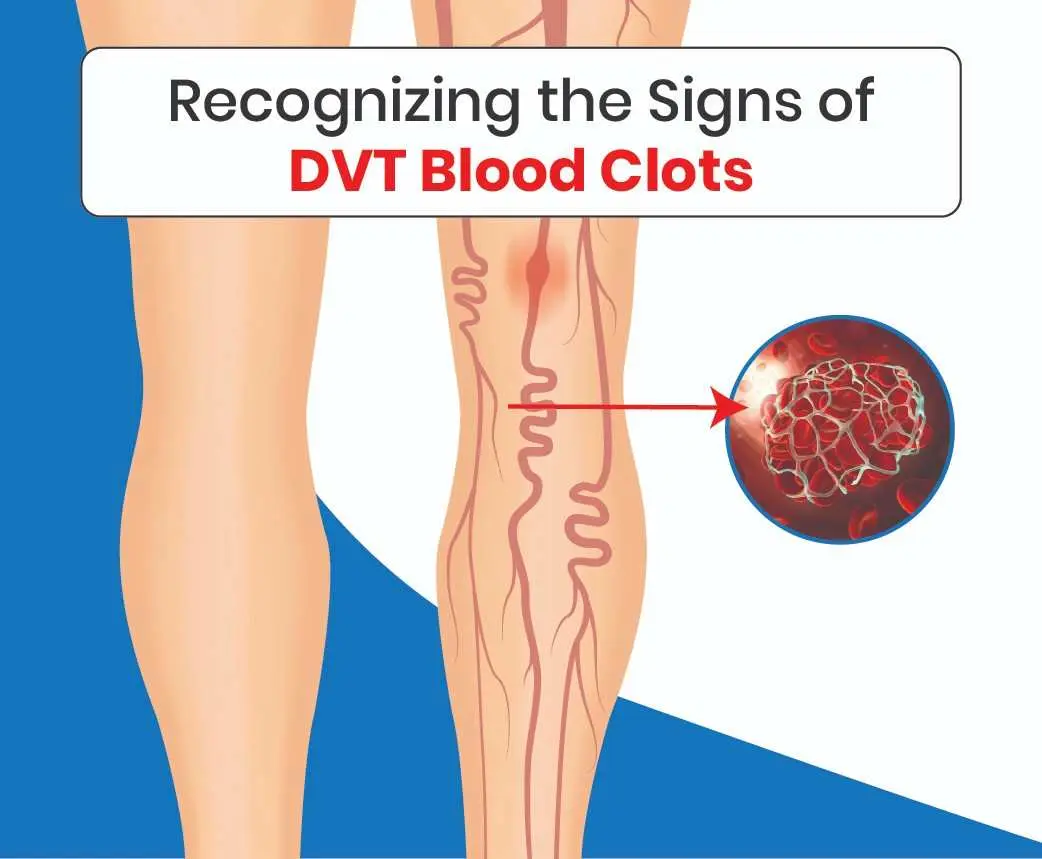
What is Deep Vein Thrombosis?
Deep Vein Thrombosis (DVT) occurs when a blood clot forms in a deep vein, usually in the lower leg, thigh, or pelvis, though they can also occur in other areas. DVT is particularly concerning because it can lead to severe complications, including death.
Causes and Risk Factors of DVT
Problems Associated with Lymphedema
DVT results from a combination of factors that affect blood flow, vein health, and blood
clotting:
Venous Stasis: Extended periods of
inactivity, such as bed rest or long flights, can slow blood flow in the legs, increasing the
risk of clotting.
Vein Damage: Injury or surgery can damage the inner lining
of veins, contributing to clot formation.
Hypercoagulability: Certain medical conditions and lifestyle choices
can make blood more prone to clotting.
Additional risk factors include obesity, Pregnancy, Cancer and its treatments. Smoking, hormonal birth control or hormone replacement therapy are other risk factors.
Recognizing DVT symptoms is crucial for timely treatment.
Identifying when a blood clot develops in your body, particularly in cases of Deep Vein
Thrombosis (DVT), involves being aware of specific symptoms. However, it’s important to note
that in some cases, blood clots can occur without any obvious symptoms. Here are key signs and
symptoms to watch out for:
DVT results from a combination of factors that affect blood flow, vein health, and blood
clotting:
Swelling: This usually occurs in one limb and is a common sign
of DVT. The swelling can be sudden and may be accompanied by pain or tenderness.
Pain or Tenderness: The pain often starts in your calf and can
feel like cramping or soreness. It might become more noticeable when you stand or walk.
Red or Discolored Skin: The skin around the painful area may become red or
discolored.
Warmth:The area around the clot may feel warm to the touch.
Leg Weakness: In some cases, there might be a feeling of weakness in the leg
where the clot is located.
Complications of DVT
Pulmonary Embolism (PE):A life-threatening condition where a part of the clot breaks off and travels to the lungs. Shortness of breath, coughing up blood, and chest pain that becomes intense while you breathe, or cough are symptoms of PE and will need immediate attention.
Post-Thrombotic Syndrome (PTS):Chronic leg pain, swelling, and skin changes after a DVT.
Red or Discolored Skin:Venous Ulcers: Long-standing DVT can lead to painful ulcers on the affected limb.
Warmth:The area around the clot may feel warm to the touch.
Leg Weakness:In some cases, there might be a feeling of weakness in the leg where the clot is located.
Frequently Asked
Questions
For any unanswered questions, reach out to our support team via email. We’ll respond as soon as possible to assist you.