Venous thromboembolism (VTE) is a condition that encompasses two related issues: deep vein thrombosis (DVT) and pulmonary embolism (PE). This condition is a significant health concern due to its potential severity and the complications that can arise if not properly managed.
Understanding Venous Thromboembolism
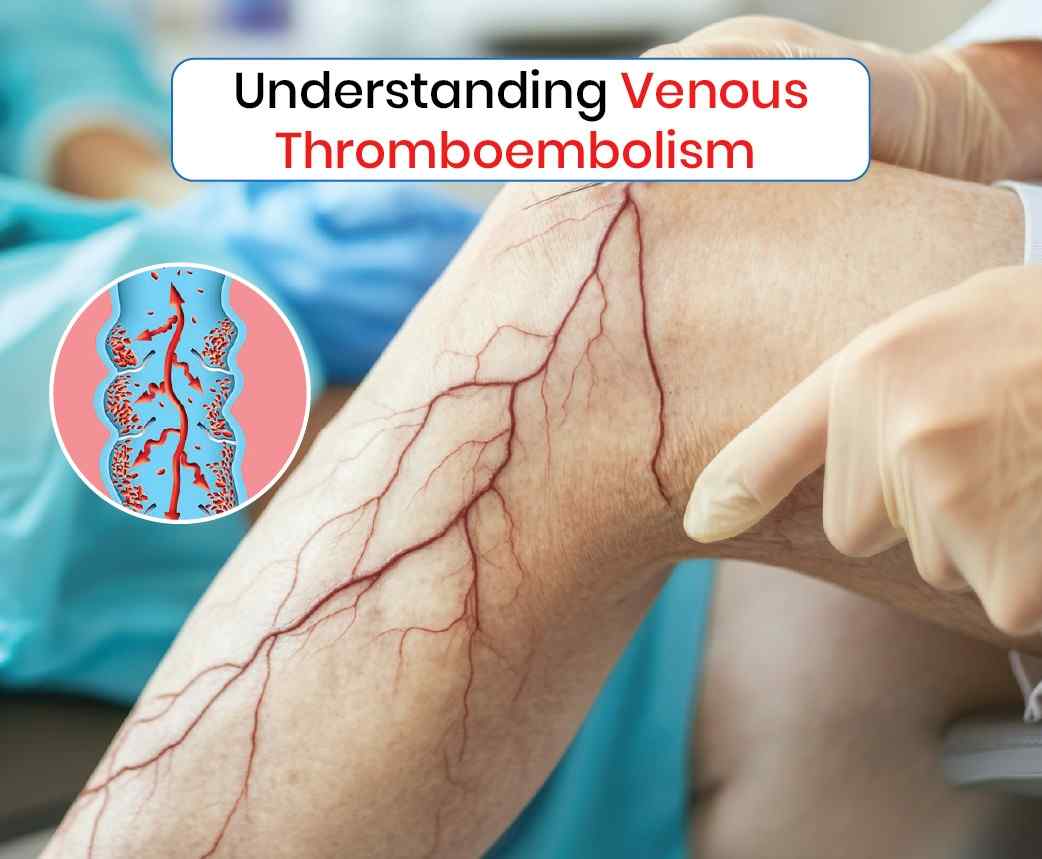
What is an Embolism?
An embolism occurs when a blood clot, air bubble, fat globule, or other substance travels through the bloodstream and lodges within a blood vessel, obstructing blood flow. This can lead to tissue damage or even life-threatening conditions depending on the location and size of the blockage.
What is Venous Thromboembolism?
Venous thromboembolism refers specifically to the formation of blood clots within the veins. There are two main types of VTE:
Deep Vein Thrombosis (DVT):
This occurs when a blood clot forms in a deep vein, typically in the legs. Symptoms might include swelling, pain, redness, and warmth in the affected area.
Pulmonary Embolism (PE):
If a part of the clot breaks off and travels to the lungs, it can cause a pulmonary embolism. Symptoms of PE include sudden shortness of breath, chest pain, rapid heart rate, and coughing up blood. PE is a medical emergency and requires immediate attention.
How Does Venous Thromboembolism Occur?
VTE can occur due to various factors that affect blood flow, blood clotting, and the structure
of blood vessels.
Key risk factors include:
Prolonged Immobility: Sitting for extended periods, such as during long flights
or bed rest, can
slow blood flow, increasing the risk of clot formation.
Surgery and Trauma: Surgical procedures and physical injuries can damage blood
vessels and
increase clotting tendencies.
Medical Conditions: Certain medical conditions, like cancer or heart disease,
can elevate the
risk of VTE.
Genetic Factors: Inherited conditions like Factor V Leiden or prothrombin gene
mutation can
predispose individuals to clotting.
Lifestyle Factors: Smoking, obesity, and certain medications (e.g., hormone
replacement therapy,
birth control pills) can also contribute to the risk.
The Importance of Treating Vein Disorders
Properly treating vein disorders is crucial in avoiding embolism. Untreated or poorly managed
vein issues can lead to the formation of blood clots, increasing the risk of VTE. For
example:
Varicose Veins: These swollen, twisted veins can lead to poor blood flow and
clot formation.
Addressing varicose veins through lifestyle changes, compression therapy, or medical procedures
can reduce this risk.
Chronic Venous Insufficiency (CVI): This condition, where veins cannot
efficiently return blood
to the heart, can lead to blood pooling and clot formation. Proper management of CVI with
compression therapy, exercise, and sometimes surgical interventions is vital.
Vein problems can lead to embolism through various mechanisms:
Blood Stasis: When blood flow slows down or stagnates, such as in the case of
varicose veins or
chronic venous insufficiency, it increases the likelihood of clot formation. Blood that pools in
the veins has a higher chance of forming clots, especially in areas where the blood vessel wall
is damaged or inflamed.
Endothelial Damage: Conditions like varicose veins or trauma to the veins can
cause damage to
the endothelium, the inner lining of blood vessels. This damage can trigger a cascade of events
that lead to clot formation, as the body attempts to repair the injured area by forming a blood
clot.
Hypercoagulable States: Certain medical conditions or genetic factors can
increase the blood’s
clotting tendency, making individuals more susceptible to clot formation. This hypercoagulable
state, combined with factors like immobility or dehydration, can significantly raise the risk of
developing blood clots within the veins.
Preventing VTE involves addressing modifiable risk factors and using medical interventions when necessary. Key prevention strategies include:
Regular Movement: For those at risk, especially during long trips or periods
of inactivity,
regular movement and exercises to stimulate blood flow in the legs are crucial.
Compression Stockings: These can help maintain blood flow in the legs and
reduce the risk of
clot formation.
Medication: Anticoagulants or blood thinners may be prescribed to individuals
at high risk to
prevent clot formation.
Lifestyle Modifications: Maintaining a healthy weight, quitting smoking, and
staying hydrated
are essential preventive measures.
Recurrence of Venous Thromboembolism
Venous thromboembolism is a serious medical condition with potentially life-threatening consequences if not properly diagnosed and managed. VTE can recur, especially if underlying risk factors remain unaddressed. Long-term management often includes continued use of anticoagulants and regular follow-ups with healthcare providers to monitor and manage risk factors. Lifestyle changes and adherence to preventive measures play a crucial role in reducing the likelihood of recurrence.
Frequently Asked
Questions
For any unanswered questions, reach out to our support team via email. We’ll respond as soon as possible to assist you.